1. The Real Business Question: Why Most Patient Apps Fail to Drive Revenue

The problem isn’t adoption alone. Downloads may spike after launch, but usage often declines sharply after the first few weeks. In many cases, the app becomes little more than a digital receptionist used only when something goes wrong or an appointment is urgently needed.
What’s missing is not functionality. It’s behavioral relevance.
Healthcare differs from consumer apps in one critical way: patients don’t open an app for entertainment or impulse. They open it when they perceive value, reassurance, or guidance. When an app fails to embed itself into a patient’s ongoing health journey, it cannot influence decisions and without influence, there is no sustainable revenue impact.
Research consistently shows that mHealth effectiveness depends on sustained engagement, not initial feature completeness. A systematic review published in JMIR mHealth and uHealth highlights that while many apps improve access, only those designed around patient behavior and long-term interaction show measurable clinical or economic benefits.
Source: https://mhealth.jmir.org
In short, most patient apps fail not because they lack features but because they lack strategy.
Key takeaway: Revenue does not come from having a patient app. It comes from shaping how, when, and why patients return to it.
2. What Research Actually Says About the Impact of mHealth Apps
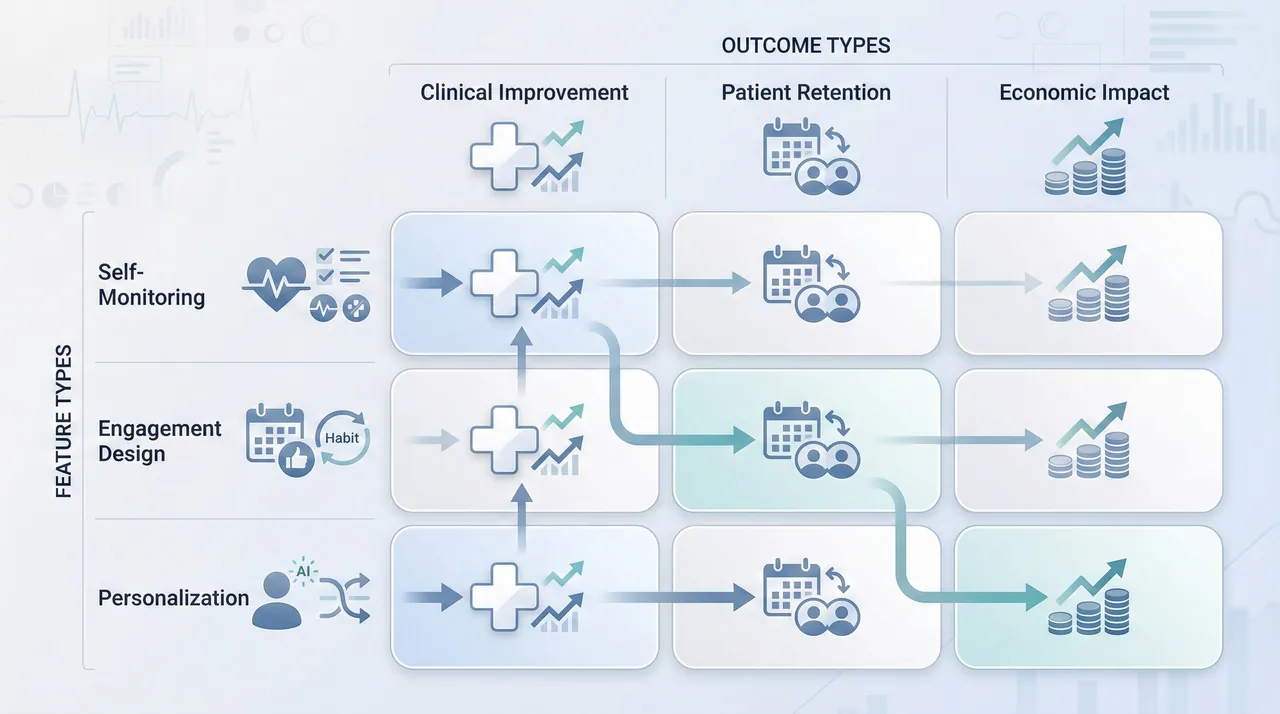
The enthusiasm around mobile health applications is not unfounded. A growing body of peer-reviewed research confirms that well-designed mHealth solutions can positively affect patient outcomes, adherence, and engagement. However, the same research also cautions against assuming universal success.
Large-scale systematic reviews indicate that mobile apps are most effective when they support self-management, continuity of care, and personalized guidance especially for chronic conditions such as diabetes, hypertension, and cardiovascular disease.
Evidence Snapshot: What Research Shows
| Research Area | Key Findings | Source |
|---|---|---|
| Chronic disease management | Improved self-monitoring, medication adherence, and symptom tracking | https://www.nature.com/digitalmedicine |
| Patient engagement | Engagement drops rapidly without behavior-driven design | https://mhealth.jmir.org |
| Clinical outcomes | Reduced readmissions and better condition control in select populations | https://pmc.ncbi.nlm.nih.gov |
| App effectiveness | Outcomes vary widely depending on usability and personalization | https://link.springer.com |
Importantly, these studies converge on a single conclusion: technology alone does not drive outcomes. The same app features can succeed in one context and fail in another, depending on how well they align with patient motivation, trust, and daily routines.
This distinction matters because revenue follows outcomes. Improved adherence reduces avoidable costs. Better engagement increases follow-up visits and continuity of care. But without thoughtful design, even the most advanced app risks becoming digital noise.
3. Engagement Is Not a Feature It’s a Behavioral System
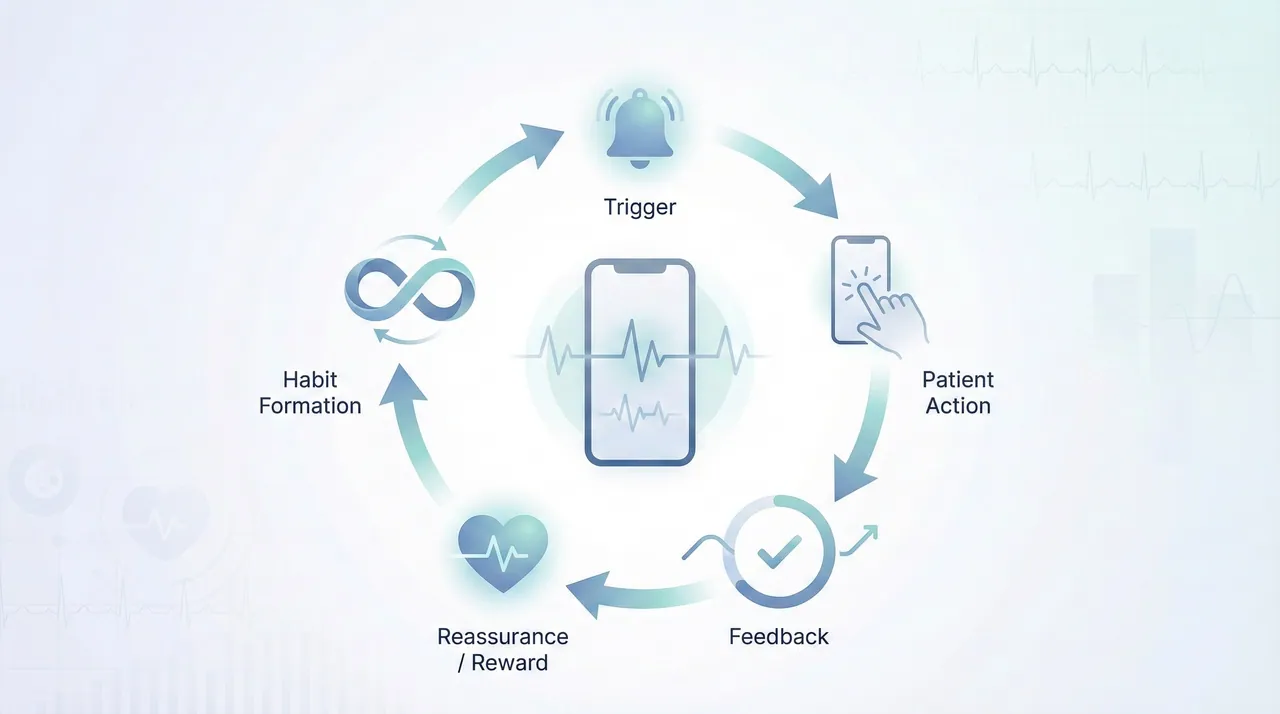
One of the most common mistakes in patient app design is treating engagement as a checklist item. Push notifications are added. Wearables are integrated. Gamification is introduced. And yet, usage remains inconsistent.
True engagement is not about novelty it’s about habit formation.
Behavioral science research shows that people repeat actions that provide immediate feedback, a sense of progress, and emotional reassurance. In healthcare, this translates into small, meaningful interactions that reinforce a patient’s sense of control over their health.
Effective engagement systems often include:
- Lightweight daily interactions (e.g., symptom check-ins)
- Visual feedback on progress (trends, milestones)
- Positive reinforcement rather than punitive alerts
- Clear personal relevance
Engagement Elements Backed by Research
| Engagement Mechanism | Behavioral Impact | Supporting Insight |
|---|---|---|
| Self-monitoring journals | Increases awareness and adherence | https://www.jmir.org |
| Wearable integration | Encourages consistency through automation | https://www.nature.com/digitalmedicine |
| Goal tracking & streaks | Builds routine without coercion | Behavioral economics research |
| Micro-rewards | Reinforces positive actions ethically | Health UX studies |
Crucially, engagement in healthcare must remain ethically grounded. The goal is not addiction, but reassurance. Patients should feel supported not pressured into returning.
When engagement is treated as a system rather than a feature, patient apps transition from reactive tools into proactive companions. And that shift is foundation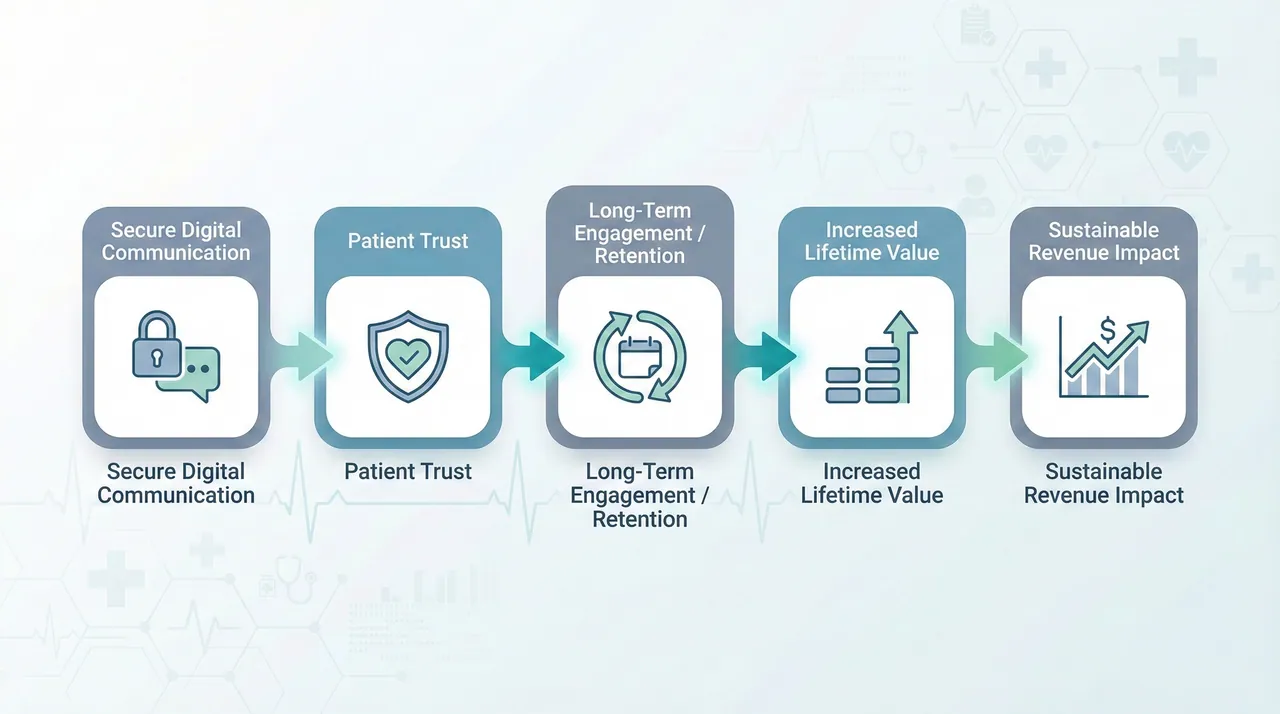
4. Trust, Retention, and the Economics of Patient Loyalty
In healthcare, trust is not a soft metric. It is a measurable economic driver.
Patients who trust a provider are more likely to follow care plans, return for follow-ups, and seek preventive services rather than episodic treatment. Digital channels amplify this effect by extending the provider’s presence beyond the clinic walls.
Research published in JMIR Human Factors and BMC Medical Informatics highlights that secure communication, responsiveness, and perceived empathy significantly influence continued app use.
Sources:
Retention has a direct financial implication. Retained patients:
- Have higher lifetime value
- Are more receptive to preventive and wellness programs
- Reduce acquisition costs over time
Trust → Retention → Revenue Chain
| Trust Factor | Patient Impact | Business Outcome |
|---|---|---|
| Secure messaging | Confidence in care continuity | Increased follow-up visits |
| Timely responses | Reduced anxiety | Higher satisfaction & loyalty |
| Personalized guidance | Perceived attentiveness | Long-term engagement |
| Transparent data handling | Privacy assurance | Lower churn |
Trust cannot be marketed aggressively. It must be demonstrated consistently through design, tone, and responsiveness. Apps that succeed financially are often those that quietly earn loyalty rather than loudly demand attention.
5. From Engagement to Monetization: Ethical Revenue Pathways
Monetization in healthcare is a sensitive topic and rightly so. Patients are not customers in the traditional sense. Any perception of exploitation erodes trust quickly.
That said, ethical monetization is both possible and necessary for digital health sustainability.
The most effective patient apps do not “sell” services. They guide decisions. By aligning recommendations with a patient’s condition, behavior, and goals, providers can promote services that feel helpful rather than commercial.
Examples of ethical revenue pathways include:
- Preventive care reminders aligned with clinical guidelines
- Personalized follow-up recommendations
- Bundled wellness or chronic care programs
- Context-aware discounts that reduce care friction
Ethical Monetization vs. Intrusive Promotion
| Approach | Patient Perception | Outcome |
|---|---|---|
| Generic pop-up ads | Distrust, irritation | App abandonment |
| Personalized care nudges | Supportive, relevant | Higher conversion |
| Preventive reminders | Proactive care | Reduced long-term costs |
| Condition-based offers | Helpful guidance | Increased service uptake |
Research in Digital Health Economics shows that personalization significantly improves acceptance of care recommendations, particularly when framed as support rather than sales.
Source: https://www.tandfonline.com/toc/ijbh20/current
The distinction is subtle but critical: patients should feel guided, not targeted.
When monetization flows naturally from engagement and trust, revenue becomes a byproduct of better care not its objective.
6. AI’s Role in Making Patient Apps Economically Viable
As patient expectations evolve, manual personalization no longer scales. This is where artificial intelligence shifts from a “future add-on” to a structural necessity.
AI’s true value in patient applications is not automation it is anticipation.
Research in Nature Digital Medicine and JMIR AI shows that predictive systems can identify patterns invisible to static workflows: missed medication risks, likelihood of appointment no-shows, or early deterioration indicators.
Sources:
Practical AI applications in patient apps include:
- Predictive reminders based on behavioral history
- Adaptive notification timing to avoid alert fatigue
- Risk-based follow-up prompts
- Conversational interfaces for triage and reassurance
How AI Improves Economic Outcomes
| AI Capability | Patient Benefit | Business Impact |
|---|---|---|
| Predictive reminders | Fewer missed actions | Reduced no-shows |
| Behavior-based personalization | Relevant guidance | Higher engagement |
| Conversational AI | Faster reassurance | Lower staff workload |
| Risk stratification | Early intervention | Cost avoidance |
Importantly, AI does not replace clinicians. It extends their reach.
7. Measuring What Matters: KPIs for Revenue-Driven Patient Apps
One reason many patient apps underperform is that success is measured incorrectly.
Downloads, daily active users, and screen time are easy to track but they reveal little about whether the app contributes to organizational goals. Healthcare leaders need metrics that connect digital behavior to clinical and financial outcomes.
Metrics That Matter
| Metric Category | Key Indicators | Why It Matters |
|---|---|---|
| Utilization | Appointment completion rate | Direct revenue recovery |
| Engagement | Long-term active users | Sustainability |
| Clinical impact | Adherence, follow-up compliance | Outcome quality |
| Economic value | Patient lifetime value (PLV) | Strategic ROI |
| Efficiency | Cost per digital interaction | Operational savings |
Studies in Health Informatics Journal emphasize aligning digital KPIs with care outcomes.
Source: https://journals.sagepub.com/home/jhi
8. Why Many Patient Apps Underperform: Common Barriers and Blind Spots
Despite good intentions, many patient apps struggle to deliver value. Research consistently highlights several recurring obstacles most of which are strategic, not technical.
Common challenges include:
- Overloaded interfaces
- Poor alignment with patient digital literacy
- Alert fatigue
- Limited integration with clinical workflows
- One-size-fits-all design assumptions
Qualitative studies published in JMIR Human Factors show that abandonment often stems from irrelevance rather than dislike.
Source: https://humanfactors.jmir.org
Barrier vs. Impact
| Barrier | Resulting Issue |
|---|---|
| Complex UI | Low sustained usage |
| Excessive alerts | Notification disablement |
| Generic content | Reduced trust |
| Poor EHR integration | Fragmented experience |
9. Designing a Sustainable Patient App Strategy
Successful patient apps are not built once; they are continuously refined.
A sustainable strategy balances clinical responsibility, patient experience, and business viability. This requires moving away from feature accumulation toward intentional design.
Four Pillars of Sustainability
- Behavior-Led Engagement
- Trust-Centered Communication
- Ethical Monetization
- Continuous Measurement & Iteration
Research in Springer Digital Health highlights the value of iterative, outcome-driven evolution.
Source: https://link.springer.com
10. The Future: Patient Apps as Continuous Care Platforms
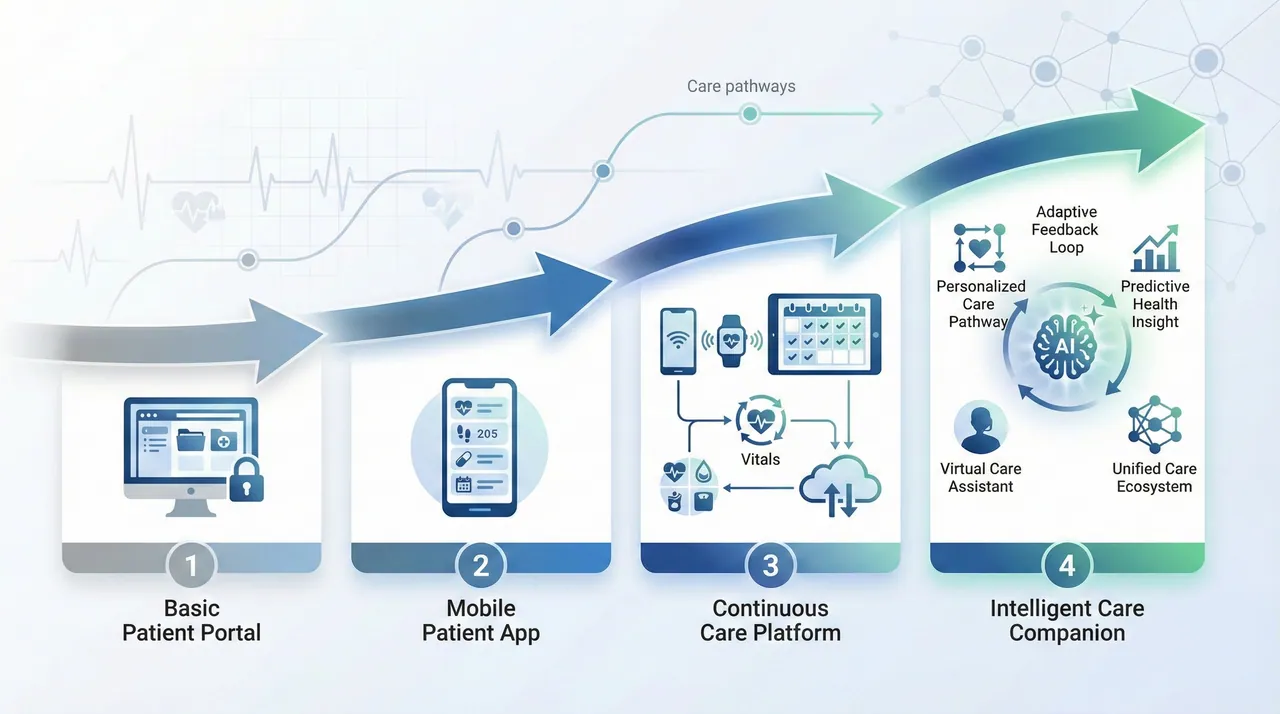
Healthcare is steadily shifting from episodic treatment toward continuous care. Patient apps are at the center of this transformation.
Future patient applications will serve as:
- Digital front doors to care
- Long-term health companions
- Data intelligence layers for providers
- Stabilizers of patient-provider relationships
A growing consensus in healthcare strategy literature suggests that future revenue will be driven not just by service volume, but by relationship longevity.
The most successful patient apps will not compete on features.
They will compete on outcomes, trust, and continuity.
For healthcare organizations willing to invest thoughtfully, mobile patient applications represent more than a digital convenience. They are an opportunity to redefine how care is delivered and how value is created ethically, sustainably, and at scale.

